Written by Dr Leigh Plowman, Optometrist (updated May 2024)
Ever have intermittent blurry or smeary eyesight?
Ever have itchy or watery eyes?
Or are your eyes sensitive and red?
Ultimate Guide Outline: what you need to know about dry eye disease and treatment.
- Common symptoms of Dry Eyes
- What is dry eye disease?
- Why are tears important for the eyes?
- What are the causes of dry eyes?
- How might dry eye affect you?
- How is dry eye diagnosed?
- Dry eye treatment
- Self-Care to prevent dry eyes
- Diet And Supplements For Dry Eye Prevention
- Medications for Dry Eye
- Dry Eye Procedures
- Book an Appointment with a Dry Eye Professional
What are the Symptoms of Dry Eyes?
Dry eye symptoms can vary from person to person.
Here is a list of symptoms you may experience if you have dry eyes:
- Sore eyes
- Blurry eyesight
- Sensitivity to wind or smoke
- Feels like something in your eye
- Irritated or gritty eyes
- Stinging or burning sensation
- Eye fatigue (i.e. your eyes are more tired than you tend to feel)
- Red eyes
- Sticky eyes
- Pain on waking or opening eye lids in the morning
- Difficulty in wearing contact lenses
- Light sensitivity or photophobia
- Difficulty in keeping your eyes open
- Watery eyes or Excessive tearing (If the normal tear quality is reduced, the body creates over-production of watery tears. It sounds odd, but dry eyes can make watery eyes.)
Here is a brief video from the American Academy of Ophthalmology:
Some of these symptoms happen regularly, and others occur intermittently. Most people’s symptoms are different, and can vary depending on whether they’re indoors or outdoors. Dry eye disease occurs when your eyes are affected at least once per day.
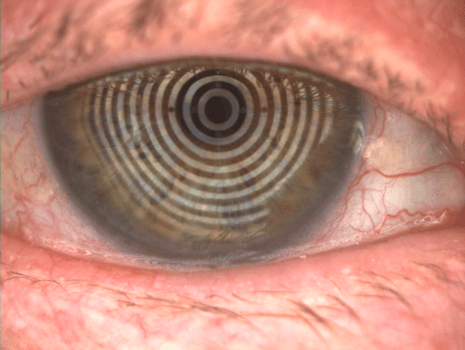
Dry Eyes causes multiple symptoms including inflammation, redness and intermittent filmy or foggy vision (Source: Dryeyedirectory.com)
Take the Dry Eye Quiz!
Do you have Dry Eye Symptoms?
Take the Dry Eye Quiz! See whether you might have dry eye.
It takes one minute or less.
Get your score instantly! Take the Dry Eye Quiz Now!
What is dry eye disease?
Dry eye disease affects the surface of the eye and results in a loss of the normal balance of things that keep your eyes comfortable and clear.
Tears spread across the cornea or the surface of the eye with every blink. The amount and quality of one’s tear are essential for one’s eyes.
At the surface of the eyes, there are many parts that work together in harmony. For example, there are muscles, nerves, glands, tear ducts, connective tissue, that all play their role in keeping the eyes moist.
Dry eye disease occurs usually when one of these factors is out of balance. This actually causes imbalance to other factors, perpetuating the cycle of dry eye disease.
“Dry eye is a multifactorial disease of the ocular surface characterized by a loss of homeostasis of the tear film, and accompanied by ocular symptoms…”
According to TFOS Dry Eye Workshop Report II (2017)
The risk of developing dry eye disease increases with age. Women are more likely to develop the condition compared with men. However, dry eye disease is becoming increasingly common in younger people with more device use like smartphones, laptops and tablets than ever before.
Increasing device and smartphone use has made dry eyes more prominent than ever before.
According to research, over 16 million Americans have dry eyes. However, this number may be significantly higher.
Those who develop the disease can experience problems with daily activities like reading, watching television, using the computer and mobile phones, dealing with work, and driving.
Why are tears important for the eyes?
Tears play an essential role in protecting and keeping your eyes healthy.
There are three types of tears – basal tears, reflex tears, and emotional tears:
- Basal tears
are the vanguard. They serve as the principal protection of the eye.
- Reflex tears
are responsible for flushing away harmful things from the eyes like dust, fumes and other harmful irritants.
- Emotional tears
are tears formed in response to great emotion like sadness, joy, anger or fear.
The right amount and quality of tears keep the eyes nourished and lubricated. Every time you blink, a protective film of basal tears spread over the surface of your eye.
Tears help with:
- Natural lubrication to reduce friction from blinking.
- Wash away unwanted stuff from the eyes
- Keeping the surface of the eye clear
- Natural proteins help fight germs or things that cause eye infection.
See how the tears are produced by the normal eye in this video
Tears have three layers – the outer lipid layer, the middle aqueous layer, and the inner mucin layer. Each layer serves a purpose.
- The inner layer is made up of mucus that coats the surface of the eye. The mucin layer binds tears to the eye. The cornea is naturally hydrophobic, so the mucous layer helps to connect watery layer above. The mucous layer is also responsible for spreading the water layer evenly over the surface of the eye.
- The middle layer which is also the thickest layer is mostly composed of an aqueous or watery layer. This layer which is more like a saline solution contains vitamins and minerals that keep the eye nourished. The watery layer is what makes up most of the tears. It is also responsible for maintaining the eye lubricated and washing away unwanted particles.
- The outermost layer of the tear is an oil or lipid-based layer. It seals the tear film, keeping the surface of the tear smooth and preventing the other layers from evaporating. In other words, the oily layer keeps your tears from drying up too quickly.
Dry eyes can occur when there is a loss of natural balance (either from external or internal problems) with any of these layers.
What are the causes of dry eyes?
There are two leading causes of dry eyes:
- rapid evaporation of tears caused by a deficiency in the oil layer (Evaporative Dry Eye or Meibomian Gland Dysfunction)
- reduction of the quantity of tears produced by the glands (Aqueous Deficient Dry Eye).
Often, there is overlap between these two main causes of dry eyes.
Several factors can affect tear production or the condition of the eye in general. Dry eyes can result from many factors, including but not limited to:
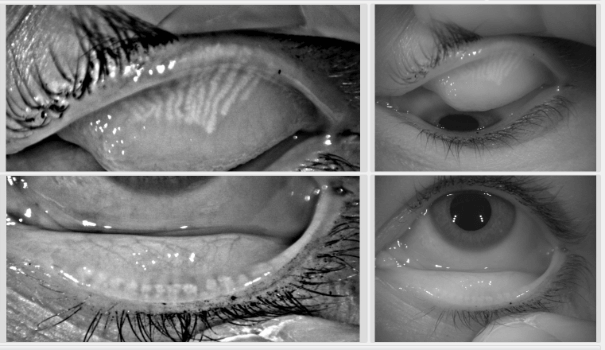
White stripes on the eyelids show the Meibomian Glands in Normal (left) vs Meibomian Gland Dysfunction (right).
- Incomplete blinking
when we concentrate on a smartphone, tablet or detailed task, we tend not to blink as often.
- Age
The amount and quality of tear the eyes produce decrease with age. Dry eyes increases in prevalence for people aged 55 and above.
- Gender
Due to hormonal changes, pregnancy, use of contraceptives and menopause, women have a higher chance of developing dry eyes.
- Cosmetics & Skincare Products
Ever tried hypoallergenic, vegan, organic or sensitive mascara? You may find ingredients that are toxic and cause dry eyes. Read more at this post. You can also learn more about Eyes Are The Story for people with Dry, Sensitive Eyes.
- Eyelid problems
conditions such as ectropion (out-turning of the lids), entropion (in-turning of the lids) can produce more exposure or friction and cause the normal tear film to dry faster.
Ocular Rosacea is one of the most common under-diagnosed causes of dry eyes. - Recent procedures
refractive eye surgery like LASIK can cause decreased tear production. This is due to a permanent change to the front surface of the eye. For some people, dry eye symptoms related to eye procedures can be temporary. Others can have persistent symptoms.
- Medications
Most medicines have side effects, and some of these can affect tear production. Medications such as blood pressure medications, antidepressants, sleeping pills, heartburn tablets, drugs for acne, birth control, hormone replacement, allergy, cold and Parkinson’s disease can reduce tear production.
- Health conditions
Autoimmune diseases like Rheumatoid Arthritis, Sjögren’s Syndrome, Scleroderma, Lupus, and Thyroid disease can directly affect the glands responsible for tear production. These conditions can cause imbalances in the three main layers of the tear – mucus, oil, and water. Vitamin A deficiency can also decrease tear production.
- Indoor and outdoor environmental conditions
Your eyes (and tears) are the most exposed parts of your body. Exposure to a dry environment, whether indoor or outdoor, can affect the eyes. People who live in places with dry climates are more prone to having dry eyes. Exposure to wind, smoke, and fumes can also aggravate your eyes. Dry indoor environments include air-conditioned rooms, hospitals, airplanes, and workplaces.
- Daily activities
Reading, staring at a smartphone or computer, driving and other similar activities require concentration leading people to blink less often which in turn causes increased tear evaporation.
- Lifestyle
Contact lenses can also irritate the surface of the eye and contribute to dry eyes. Other activities like cigarette smoking, alcohol consumption and not getting enough sleep can also affect the dryness of your eyes.
How might dry eye affect you?
Dry eye disease is a condition that is often overlooked but can have serious short term and long term effects on those who develop it.
Short term effects include constant eye irritation, blurry vision, regularly tired eyes and difficulty in wearing contact lenses.
Dry eyes can start out as uncomfortable and annoying, but more than that it can cause permanent vision impairment if not taken care of and managed well.
Dry eyes can also impact the way you usually live your life. People may face lifestyle restrictions. Simple daily activities like reading, working and driving can become difficult.
Dry eyes can also get in the way of productivity in work and non-work related activities. Dry eyes can even impact quality of life.
Therefore diagnosing and treating dry eye disease during its early stages is essential.
Join the Dry Eye Care Group on Facebook
How is dry eye diagnosed?
A person must go under tests and procedures to determine what’s causing their dry eyes. Each case can be different and may require custom treatment.
Your optometrist or ophthalmologist will start with an eye exam. Tests and evaluation may include one or more of the following.
A comprehensive eye exam notes a patient’s complete health history and lifestyle that maybe the underlying cause of the dry eyes. It also involves examination of the eyelids and the surface of the eye.
An assessment of the tears that measures the volume and quality of tears helps determine whether there is a deficiency in your tear quantity or quality.
In this assessment, your eyecare professional will be able to decide on how quickly the eye produces tears and how long it takes for them to evaporate.
Here is an example showing how the tears start to evaporate in some locations before others:
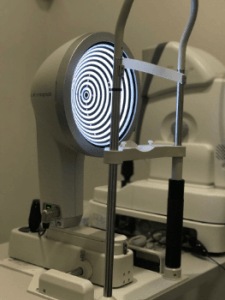
The Oculus Keratograph is used to measure tear quality and stability (Source: Dryeyedirectory.com)
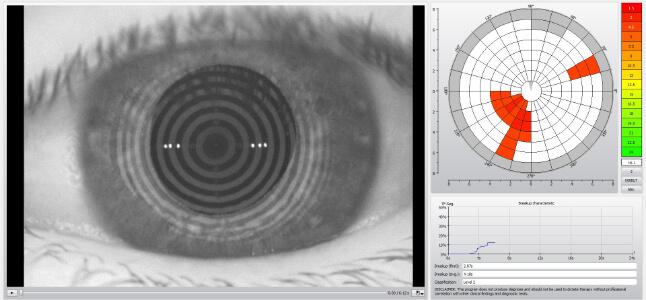
Tear breakup time showing the areas of the eyes that evaporate fastest (in red) (Source: Dryeyedirectory.com)
Examining a tear sample under a microscope can also help diagnose if there’s any inflammation associated with your symptoms.
This diagnosis may include examinations like Schirmer test where blotting test strips of paper are placed on the lower eyelids to determine the volume of tears the eye produces at a certain amount of time.
There’s also the Epithelial staining that uses a particular eyedrop with a yellow dye that helps determine how quickly the tears dry out. You’ve probably had this dye put in your eyes before. It also helps identify if there’s any damage in the surface of the eye.
Meibomian Gland Evaluation, on the other hand, helps determine if the Meibomian glands are producing enough oil to keep the eye lubricated.
Your optometrist or ophthalmologist then helps you to form a plan with the most applicable treatment to help your eyes.

A Meibomian Gland Evaluator helps to evaluate how much oil is produced. (Source: Dryeyedirectory.com)
Dry Eye Treatment
How can you treat dry eyes?
Dry eyes are often managed, rather than cured. However, research and technology have given us significant improvements. Importantly, these can make a big difference to your quality of life.
Self-Care to prevent dry eyes
If you’re looking to do yourself a favour, here are some tips you may want to consider:
- Blink more often
avoid staring at computers and phones for an extended period. Make a conscious effort to rest your eyes in regular intervals, such as every twenty minutes. These are especially important when your daily activities require you to use smartphones and devices. Blinking exercises can really help, especially after you use a warm compress or Blephasteam treatment. Here’s how to do your blink exercises
- Remove eye makeup like eyeliner, mascara foundation, and eye shadow thoroughly. Check the ingredients on your makeup carefully. Too many people buy makeup based on what’s on special. However, chemicals in some makeup can damage your Meibomian Glands and surface of your eyes. Look for makeup without these ingredients. Don’t silently cause damage to your eyes.
- Prevent dry eyes overnight
Sometimes the eyes don’t fully shut overnight. This leads to air exposure and dryness. Eye masks such as Tranquileyes are silicone eye masks which prevent evaporation overnight. They’re not just suited for people who use a CPAP machine, but anyone with sore eyes upon waking.
- Dry Eye Glasses
Dry Eye Glasses can give you relief from dry eyes in minutes. They wrap-around your eye sockets and can block the sun’s UV-A and UV-B rays . Importantly, they also protect your eyes from hot or cold wind, dust and other particles. With reduced evaporation, your eyes naturally feel more comfortable after wearing dry eye glasses. You can also get clear lenses (with or without your prescription in them), and they can make a big difference with air conditioning at work.
- Invest in a humidifier for your home or workplace to add moisture to the air.
- If you have an allergy that causes your eyes to itch, use preservative-free antihistamine eyedrops to prevent them from itching. Reduce eye rubbing too so that you don’t create more inflammation and dryness.
- Don’t overwear your contact lenses…
for too long. Always keep them clean and never forget to take them out at night. Wear daily disposable lenses to prevent bacterial buildup and keep your eyes feeling fresh.
- Reduce Cigarette Smoking
Cigarettes contain hundreds of toxic chemicals that inflame and damage your eyes. Industrial chemicals, smoke and fumes can also affect your eyes. Make sure your eyes are protected from the environment you work in.
- Apply warm compresses to your eyes. Some are easy to heat and re-use. Some are washable. Some people use a boiled egg that has cooled enough to be touch comfortably. Don’t massage your eyes- instead leave it to your eyecare professional to clear any blocked oil glands.
Specific diets and supplements can also help keep your eyes nourished and treat dry eyes.
Diet And Supplements For Dry Eye Prevention
Eating healthy helps ensure your eyes get the vitamins and minerals they need. To protect your vision, improve overall eye health and relieve your dry eyes symptoms, you may want to start adding vital nutrients to your diet.
- Water
it’s easy to say, but keeping your hydration levels up can help improve the comfort of your eyes. It’s great for your skin, bowels, kidneys and your eyes.
- Omega-3 fatty acids…
Omega-three is an anti-inflammatory and building block for Meibomian Gland Oil. Fish, leafy vegetables, vegetable oil, soybeans, nuts, and seeds are good sources of omega-3s. Fish oil supplements may also help.
- Vitamin D supplementation
if you’re someone who works indoors, it’s easy to not get enough Vitamin D. Not only can this affect your bones. It can also affect your eyes. New studies are showing that Vitamin D supplementation (e.g. cholecalciferol) can improve the effectiveness of artificial tears on the eyes.
- Vitamin A
helps protect the surface of the eye. Vitamin A deficiency can increase dry eyes. Add food rich in Vitamin A to your diet, like carrots, fortified skim milk and other orange and yellow fruits and vegetables. Eye drops with vitamin A can also be an effective treatment for dry eyes.
- Zinc
also plays a significant role in keeping the eye healthy. It’s the mineral responsible for getting vitamin A from your liver to your retina and producing melanin, a pigment that protects your eyes. Dairy, whole grains, nuts, legumes, and meat are excellent sources of zinc.
- Lutein and zeaxanthin
are antioxidants that help keep cells healthy and functioning correctly. They help prevent many chronic eye diseases like dry eyes. Foods rich in these antioxidants include leafy greens like spinach, kale, romaine lettuce and silver beet. Supplements with lutein and zeaxanthin can also be an option.
- Intestinal Microbiome
(i.e. gut bacteria)- research is showing the emerging role of the intestinal microbiome can affect multiple body systems. If you’re taking Omega-3 supplements, your microbiome may influence absorption of omega 3 into your body. Talk to your Primary Doctor or Naturopath about a test of your microbiome.
Always remember that it’s best to consult your doctor or healthcare professional before taking any supplements.
Medications for Dry Eye
There are several over-the-counter and prescription eye drops that can help with dry eyes. Remedies for dry eyes may include the following:
- Manuka Honey Eye Drops
(e.g. Optimel Drops) not only help lubricate your eyes, but they are also a natural antibiotic/anti-inflammatory. Despite an intial sting, the drops feel soothing within minutes of putting them in. Many people find relief for dry eyes from this naturally derived product. As of writing, Manuka Honey drops are available in the United Kingdom and Australia. However, they are also available on online (e.g. Amazon).
- Eyelid wash
can reduce eyelid inflammation. This is also known as Anterior Blepharitis or just Blepharitis. Hypochlorous acid wash (e.g. Avenova) or tea tree foams (e.g. WeLoveEyes, Cliradex*) help to reduce the quantity of bacteria & eyelid mites that live near your eyelids and lashes. This helps reduce the number of bacteria that throw toxins into your eyes and make them drier. They also help your eyes feel fresher. The best time to use the wash/foams is at night.(*affiliate link- view affiliate disclosure here)
- Nulids
Want to get relief at home? Nulids is an at-home treatment. It takes about one minute per day. A recent study found that it works by cleaning your eyelash area and improve clogged oil glands. Most people reported that they were satisfied with their treatments. Tap here to learn more about Nulids.
- Artificial tears
are probably the most common medication to dry eyes. It helps lubricate the eyes and treat irritation, dryness, and inflammation. While it can relieve some of the common symptoms, it will not be able to deal with the underlying cause of dry eyes. Look for preservative-free drops, especially when using multiple drops, or using them more than four time per day. Good drops like Hylo-Forte and Novatears are very useful together, but you need to instill them about five minutes apart, so they don’t dilute. Use Novatears last because it’s an oily drop and you want to keep this oily layer on top.
- Prescription eye drops
that contain immune-suppressing medication (Xiidra, Restasis, Cequa, Ikervis) or corticosteroids can help relieve inflammation in the cornea. Restasis and Xiidra normally take a period of time to take effect. Topical corticosteroids (e.g. fluormetholone, FML, Flarex) are usually used in short term doses to rein in inflammation. Unlike artificial tears, this medication requires a prescription.
- Eye ointments
do you ever have sore eyes when you wake up? Sometimes you can have a small gap between your eyelids overnight. This is called Lagophthalmos and can lead to exposure and dryness. Eye ointments (e.g. VitaPos), give soothing relief to your eyes overnight. It contains Vitamin A.
- Hydroxypropyl cellulose ophthalmic inserts or eye inserts
work the same way as artificial tears, but the application is different. The insert is placed between the lower eyelid and the eyeball. It is like a transparent grain of sort which dissolves slowly and provides artificial lubrication to the eye. Eye inserts are another option when artificial tears solution are not successful.
- Cholinergic drugs
are drugs that can be used to stimulate tears. This medication helps increase tear production. However, side effects have limited widespread use of these drugs.
- Autologous blood serum drops
or eyedrops made from your blood serum and plasma are a standard option when other treatment does not work. The blood is processed and mixed with sterile saline. It is a well-known remedy for severe cases of dry eyes. This eye drop contains components present in natural tears, which make it an ideal treatment for dry eyes. However, there are no preservatives and it must be kept refrigerated.
- Hormone Replacement Therapy
some women may benefit from HRT if menopause is the underlying cause. However, for other women, HRT may also cause dry eye. Check with your Primary Care Doctor (or General Practitioner) to see if HRT may help you.
- Nasolacrimal Stimulation
Tyrvaya and iTear100 are treatments that switch on more natural tears. They help activate more tears (not just the watery layer, but oily layer also). Dosing is approximately twice per day. Tap here to learn more
It’s always best to have your eyes examined before trying any medication, especially if the medicine makes direct contact to the eyes. The wrong drug might make your eye condition worse.
Dry Eye Procedures
If eye drops and medication don’t work, procedures may be used to treat dry eyes. Treatment will be different for each person depending on the root cause of the dry eye. Some of these procedures require a series of treatments to achieve results. They may also require maintenance sessions. Dry Eye Procedures include:
- Meibomian Gland Expression
can also help open up clogged Meibomian glands. Eyelid glands are typically warmed gently with a special type of goggles (e.g. Blephasteam). Soon after, your eyecare professional may gently express/clear any clogged glands. This helps clear oil to come through underneath. Lipiflow is an automated heating and expression system done in-office.
- Intense Pulsed Light (IPL) treatment
uses light therapy to liquify oils that may have hardened and clogged the Meibomian glands. It uses visible light and infrared. IPL Dry Eye can help fade sunspots or spider vessels on the face. For the eyes, IPL helps reduce inflammation around the face and eyelids and improves Meibomian Gland function. IPL is often followed by Meibomian Gland Expression.
- Punctal occlusion
is a procedure that can permanently or temporarily close off the tear drainage, allowing the eyes to retain the tears much longer before they evaporate. However, punctal occlusion may also increase inflammation, so your eyecare professional will weigh up the benefits of punctal plugs with you. - Scleral contact lenses
are special contact lenses that help trap moisture in the eyes. The space between the cornea and the surface of the scleral lenses serves as a fluid reservoir, keeping the eyes moist. These lenses are one of the standard remedies for severe cases of dry eyes. In fact, Tom Cruise used Scleral Lenses in the movie, Mission Impossible:Rogue Nation, to keep his eyes open while hanging onto the side of the plane! Tap here to watch. - Amniotic membranes and drops
these are like ocular surface bandages. Amniotic membranes contain a rich supply of anti-inflammatories and natural growth hormones. Membranes can be placed over the eyes, like a contact lens, to promote healing of the ocular surface. One example is from Prokera. Amniotic eyedrops are also being formulated with similar properties. These can significantly reduce inflammation in dry eyes. Early studies have shown a significant difference in early results.
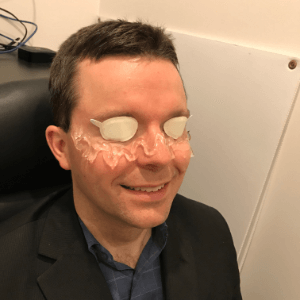
Intense Pulsed Light (IPL) setup showing stickers and gel prior to treatment. (Source: Dryeyedirectory.com)
Want to connect with other people with Dry Eyes?
Join the Dry Eye Care Group on Facebook
The Key Takeaway: Your eyes are important. Dry Eye Treatment is a must.
Dry Eye Disease is increasingly common. Without proper treatment, dry eye disease that can affect how you live your daily life.
Treatment should be sought early to avoid atrophy (i.e. shrinkage and loss of function) of the glands. Once the glands atrophy, dry eye disease is often irretrievable and makes management difficult.
Visit an optometrist or ophthalmologist to ensure you have a personal treatment plan designed for you.
Don’t wait for dry eyes to get worse before you take action.
Book an appointment with your local Dry Eye Professional. Find someone who can take the first step with you, and walk with you on the journey! Locate my nearest dry eye clinic

